Ava’s Story
Ava was the runt of the litter by a large margin; she was consistently 3-4oz smaller than her siblings even though she ate well. It was a celebration when she broke the one pound mark at nearly 9 weeks! She remained small and slender as she grew and earned the nickname “Noodle”. By 11 months she had just tipped over twelve pounds.
Once her heat cycle started her appetite was significantly reduced, which is pretty normal in my experience. Her cycle was shorter than expected (we later learned she had a split cycle) yet her appetite remained suppressed. After a couple weeks of poor appetite and mild lethargy we decided to have blood work done, just to make sure.
It came back with some anomalies so she was put on a course of antibiotics and scheduled for a recheck two weeks later. The second blood panel showed the same anomalies and it was concluded that the most likely culprit was either Addison’s disease or a liver shunt. We ordered bile acids and cortisol tests, and a board-certified radiologist performed an ultrasound on Ava’s liver. She was unable to definitively diagnose but it looked like Ava had a porto-azygos liver shunt. We also discovered that Ava had lost two pounds, putting her at only ten pounds.
We got the blood test results on June 3, Ava’s first birthday. They were definitive for a liver shunt: normal range for bile acids is in the tens of µmol/L and Ava’s was in the hundreds. We immediately started coordinating abdominal surgery and she was scheduled for June 7 with two board-certified veterinarians (one our own vet, the other visiting). They placed an ameroid constrictor on her vena porta and the casein lining on the ring would gradually close over the next 4-6 weeks to redirect blood through her liver. She recovered exceptionally well and within 4 days was bored out of her noggin, which was unfortunate since she had staples for two weeks and was on strict rest.
Do you know how hard it is to keep a terrier on strict no jumping, walking only bed rest? Ugh. We tried a sedative once but it had no effect so we resigned ourselves to another ten days of hawk-like supervision.
A Few Facts
There are two categories of liver shunts: intrahepatic (IHPSS, in the liver) and extrahepatic (EHPSS, outside the liver). Ava’s was extrahepatic, which was fortunate since intrahepatic has a much poorer prognosis. IHPSS is more common in large breeds whereas EHPSS is more common in small breeds. In one study of Cairn terriers the overall prevalence in a population of 6,367 dogs was 0.58%. EHPSS is congenital, which means it’s an embryonic developmental anomaly. There is a strong argument for it being inherited as a complex polygenic genetic trait although researchers don’t yet know exactly what genes cause it.
In an unaffected dog, blood transfers nutrients, toxins, and bacteria from the digestive tract to the liver via the portal vein. The liver then filters the blood before sending it back to the systemic blood stream to be circulated throughout the body. In a dog with EHPSS the blood never goes through the liver and instead is dumped, unfiltered, into the systemic blood stream. This leads to hepatic atrophy (small liver size) and eventually the buildup of toxins leads to death.
While it can be diagnosed as early as 6 weeks of age, many dogs aren’t diagnosed until 2-4 years of age. By that time the toxins have reached a level at which they’re causing neurological symptoms such as seizures. We were extremely fortunate to catch Ava’s shunt at all since she was almost entirely asymptomatic. Surgery is the only treatment and fortunately the prognosis for EHPSS is excellent.
Here are a few links with excellent info
- Journal article in Mammalian Genome
- Paper by the recognized expert on liver shunts
- Info at the American College of Veterinary Surgeons
Looking Forward
Pre-surgery weight: 10.5lb
Bile acids: pre-meal 177.5 µmol/L (normal <13), post-meal 318.9 µmol/L (normal <25)
2mo post-surgery: 14.8lb
Bile acids: pre-meal 1.8 µmol/L, post-meal 96.2 µmol/L
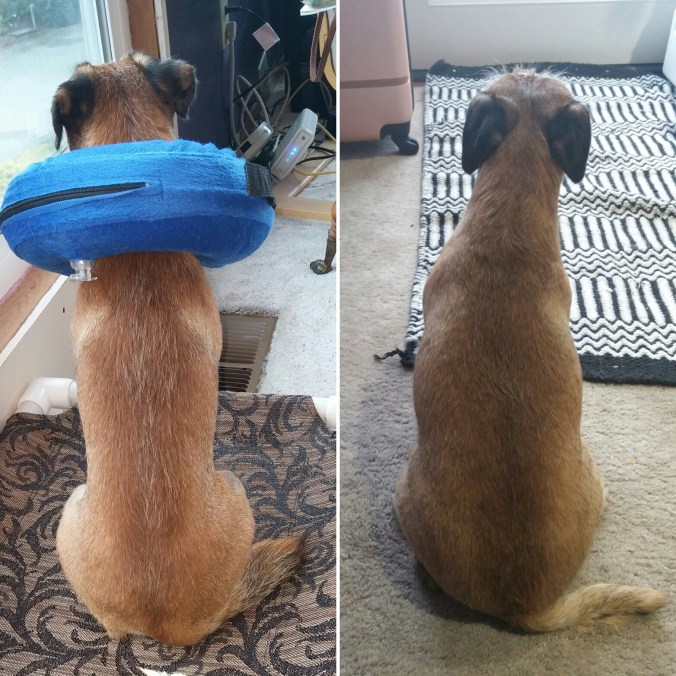
June 2017 (left) compared to Dec 2017; a 6lb weight gain!
Two months post-surgery Ava is no longer a slender, floppy noodle! Her appetite has improved, she has a LOT more energy, and she’s much more of a spitfire. Her bile acids, while still high post-meal, are significantly lower and should continue to decrease over time. We expect her to live a normal lifespan with no residual effects and her liver should regenerate as well. She has a whole new lease on life!
Her littermates were also tested and Ava was the only puppy affected in the litter. Theoretically the risk of passing EHPSS on to her offspring is low, but it would be unethical to breed a dog who had this condition. She’ll be spayed. While initially disappointing, we’ve decided to see it as an opportunity. At some point in the next few years we’ll consider adding another female to our little family but for now we’re just grateful that Ava is alive and thriving.






